SCI Pamphlets: Staying Healthy after a Spinal Cord Injury
The pamphlet series:
• Taking Care of Pressure Sores
• Maintaining Healthy Skin (Part I)
• Maintaining Healthy Skin (Part II)
• Taking Care of Your Bowels: The Basics
• Taking Care of Your Bowels: Ensuring Success
Taking Care of Pressure Sores
[Download this pamphlet: "Taking Care of Pressure Sores" - (PDF, 527KB)]
A pressure sore is any redness or break in the skin caused by too much pressure on your skin for too long a period of time. The pressure prevents blood from getting to your skin so the skin dies. Normally the nerves send messages of pain or feelings of discomfort to your brain to let you know that you need to change position, but damage to your spinal cord keeps these messages from reaching your brain.
You may need to learn new ways to change your position to prevent too much pressure. Pressure sores can occur, for example, when you sit or lie in one position too long. Shearing is also a kind of pressure injury. It happens when the skin moves one way and the bone underneath it moves another way. An example of this is if you slouch when you sit.
Another type of injury, an abrasion, can occur when pulling yourself across a surface instead of lifting. This is an example of a friction injury. In addition, short exposure to high pressure, such as a bump or fall, may cause damage to the skin which may not show up right away.
Stages of pressure sores and how to care for them:
STAGE ONE
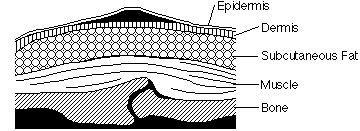
How to recognize: Skin is not broken but is red or discolored. The redness or change in color does not fade within 30 minutes after pressure is removed.
What to do:
-
Keep pressure off the sore!
-
Maintain good hygiene. Wash with mild soap and water, rinse well, pat dry carefully (but gently). Do not rub vigorously directly over
the wound. -
Evaluate your diet - are you getting enough protein, calories, vitamins A and C, zinc and iron? All of these are necessary for healthy skin.
-
Review your mattress, wheelchair cushion, transfers, pressure releases, and turning techniques for possible cause of the problem.
-
If the sore seems to be caused by friction, sometimes a protective transparent dressing such as Op-Site or Tegaderm may help protect the area by allowing the skin to slide easily.
-
If the sore does not heal in a few days or recurs, consult your health care provider.
STAGE TWO

How to recognize: The epidermis or topmost layer of the skin is broken, creating a shallow open sore. Drainage may or may not be present.
What to do: Follow steps 1-4 under Stage One. Consult your health care provider for further treatment, which may include the following:
5. Cleanse the wound with water or saline solution and dry carefully. Apply either a thin foam dressing (such as Allevyn), a hydrocolloid dressing (such as DuoDERM), or saline dampened gauze. The first two types of dressing can be left on until they wrinkle or loosen (up to 5 days). If using gauze, it should be changed twice a day and should remain damp between dressing changes.
6. Check for signs of wound healing with each dressing change.
7. If there are signs of infection (see Signs of Trouble , below), consult your health care provider for alternative wound care ideas and review of possible causes (see step 4 under Stage One).
STAGE THREE
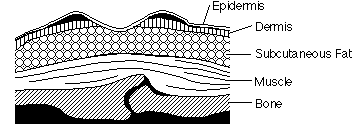
How to recognize: The break in the skin extends through the dermis (second skin layer) into the subcutaneous and fat tissue. The wound is deeper than in Stage Two.
What to do: Follow steps 1-4 under Stage One and 5 - 7 under Stage Two. Always consult your health care provider. Wounds in this stage frequently need additional wound care with special cleaning or debriding agents. Different packing agents, and occasionally, antibiotics (creams or oral pills) may be required. You may also qualify for a special bed or pressure-relieving mattress that can be ordered by your health care provider.
STAGE FOUR
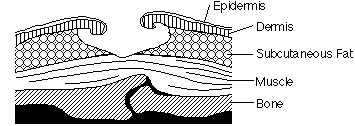
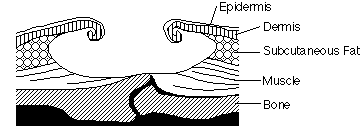
How to recognize: The breakdown extends into the muscle and can extend as far down as the bone. Usually lots of dead tissue and drainage are present.
What to do: Consult your health care provider right away . Surgery is frequently required for this type of wound.
How to know if the sore is healing
- The sore will get smaller.
- Pinkish tissue usually starts forming along the edges of the sore and moves toward the center; you may notice either smooth or bumpy surfaces of new tissue.
- Some bleeding may be present. This shows that there is good blood circulation to the area, which helps healing.
Signs of trouble
You need to seek help if any of the following occurs:
- An increase in the size or drainage of the sore.
- Increased redness around the sore or black areas starting to form.
- The sore starts smelling and/or the drainage becomes a greenish color.
- You develop a fever.
What kind of complications can be caused by pressure sores?
- Can be life threatening.
- Infection can spread to the blood, heart, bone.
- Amputations.
- Prolonged bed rest.
- Autonomic dysreflexia.
Reapplying pressure:
Only when a pressure sore is completely healed can pressure be reapplied over the area. Complete healing means that the outer layer of skin (the epidermis) is unbroken and normal coloring has returned to the area. Sometimes a scar may remain. A scar is healed tissue but will remain a somewhat different color from the surrounding skin. Scar tissue is never as tough as uninjured skin.
The first time pressure is applied to a newly healed area, it must be for a very short time (15 minutes at most). Then remove pressure from the area and inspect it for redness (erythema).
If there is redness, observe it and time carefully how long it takes to fade to the color of the surrounding tissue (or the color it was before the pressure was applied in the case of a scar). If fading occurs in 15 minutes or less, no damage has occurred. Wait at least one hour and repeat pressure application.
After three successful 15-minute trials, increase to 30 minutes and repeat the above process using the guideline of a 15-minute or less fading time as a successful trial. After three successful 30-minute trials, you may increase the time by 30 minutes each day.
If at any point a trial is not successful, hold at that level until three successful trials are accomplished. In this way, you will rebuild your skin pressure tolerance.
University of Washington-operated SCI Clinics:
Harborview Medical Center
Rehabilitation Medicine Clinic
325 9th Ave., Seattle WA 98104
Spinal Cord Injury Clinic nurses: 206-744-5862.
University of Washington Medical Center
Rehabilitation Medicine Clinic
1959 NE Pacific, Seattle WA 98195
Spinal Cord Injury Clinic nurses: 206-598-4295






