SCI Statistics from the Model Systems
As one of the 16 Model Spinal Cord Injury (SCI) Care Systems funded by the U.S. Department of Education, the Northwest Regional Spinal Cord Injury System (NWRSCIS) at the University of Washington collects medical and other data on people with SCI, starting at the time of injury and continuing with periodic follow-up questionnaires over 25 years. If you are part of this follow-up study, you may be wondering what we do with all that information.
Since the early 1970s, SCI centers such as ours have been sending SCI patient data to the National Spinal Cord Injury Statistical Center (NSCISC; http://www.spinalcord.uab.edu ; 205-934-3330) in order to monitor trends in injury (such as cause, severity, age, etc.) and evaluate the effectiveness of services and treatments. Over the years, this information has contributed to the improvement of SCI care around the nation and the world. 1
As of November 2003, the National SCI Database contained information on 22,599 patients, 1,028 of whom came from our center here at the University of Washington. The following information is drawn from the NSCISC's SCI Facts and Figures at a Glance (December 2003) and the 2003 Annual Report for the Model SCI Systems.
Age at Injury
The average age at the time of injury has increased nationally, from 28.7 years before 1979 to 37.8 years since 2000, reflecting a corresponding increase in the average age of the U.S. population. The occurrence of SCI is highest in the 16-30 age group, which accounts for more injuries than all other age groups combined.
Etiology (Cause of Injury)
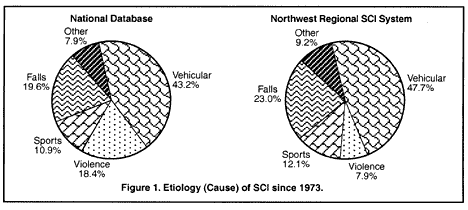
Motor vehicle accidents (MVAs) have been the leading cause of injury nationally for the last 30 years (see figure 1), but the percentage of injuries due to MVAs has declined gradually, from 47% before 1979 to 40.2% in 1999. Injuries from falls-the second most frequent cause-has increased steadily from 14.3% to 23.2% during this same time. Injuries from violence (mostly gunshot wounds) also increased, temporarily taking second place in the mid-1990s, and have subsequently declined. Sports injuries decreased from 14.3% to 7.0% between 1973-99, partly due to better prevention measures.
Etiology varies significantly by age. For example, in the 16-30 age group, falls are responsible for 10.7% of injuries and violence accounts for 22.8%. Among 46-60-year-olds, however, 36.8% of injuries are due to falls and only 8.8% to violence.
Gender and Race
Nationally, 81.3% of all injuries occur among males (78.2% in the NWRSCIS). While most injuries overall occur among whites, the percentage has decreased steadily: in 1973-77, 76.8% of persons injured were white; in 1992, 62.8% were white. This partly reflects trends in the U.S. population, but there also have been changes in the race-specific rates of occurrence.
Occupational Status
The impact of SCI on employment is striking. At time of injury, 63.8% of patients were employed, while 15.3% were students and 16.7% were unemployed. One year post-injury, however, only 13.8% were employed (15.6% among persons with paraplegia, 13.0% among those with tetraplegia) . This gradually increased to 43% (paraplegia 46.1%; tetraplegia 41.7%) by year 25, but never achieved pre-injury levels.
Neurologic Level and Completeness of Injury
The majority of patients in the database had cervical lesions (50.9%), 34.7% had thoracic, and 10.8% had lumbo-sacral lesions. The most common lesion levels were C5 (14.7%), C4 (13.6%), C6 (11%) and T12 (6.9%).
The percent of patients with incomplete injuries increased from 45.9% in 1973-79 to 55.8% in 2000-03, partly due to the introduction of high dose methylprednisolone as standard therapy within hours after injury. Incomplete injuries declined briefly between 1991-94, due to a corresponding increase in SCIs caused by gunshot wounds, which are usually complete.
Level and severity of injury varies according to etiology. For example, most (88.1%) injuries from sports accidents, but only 29.1% from violence, result in tetraplegia. Incomplete tetraplegia is the most common injury for all etiologies-except for acts of violence, which most often result in complete paraplegia.
Length of Hospital Stay
The average length of stay (LOS) in the hospital following injury has decreased significantly in the last 30 years (see Table 1) as medical care has improved and insurance coverage has become more stringent. This decrease is seen in both acute and rehabilitation LOS.
Average Number of Days in the Hospital Following Injury |
||||||
Year |
National |
NWRSCIS |
||||
| Acute | Rehab | Total | Acute | Rehab | Total | |
| 1974 | 25 | 115 | 140 | 26 | 181 | 207 |
| 1990 | 18 | 65 | 83 | 26 | 66 | 92 |
| 2000 | 18 | 46 | 64 | 15 | 46 | 61 |
Average acute and rehab LOS were longer for persons with tetraplegia than those with paraplegia. This difference is small for acute LOS but substantial for rehab LOS. Likewise, neurologically complete injuries usually resulted in longer acute and rehab LOS.
Model SCI System Research Studies
The Model SCI Care Systems also receive funding to conduct individual and multi-center research projects, and these have played a major role in raising the standard of SCI care and advancing new treatments in the past 30 years. 2
Research studies in the 1970s emphasized acute care and survival immediately after injury and contributed to significant improvements in traumatic SCI care. In the 1980s research efforts focused on prevention and treatment of common medical complications, such as pressure ulcers and urinary tract infections, and on more rigorous research designs and clinical trials. In recent years, innovative studies have evaluated new drugs and biotechnical developments. (For information about studies conducted by the NWRSCIS, see the Summer 2003 issue of the SCI Update newsletter.)
For More Information
Find out more about the 16 Model SCI Systems by visiting the Model SCI System Web site or by calling the National Center for the Dissemination of Disability Research at 800-266-1832.
References
- Tate D and Forchheimer M. Contributions from the Model Systems Programs to Spinal Cord Injury Research J Spinal Cord Med 2002;25:316-330).
- Ditunno JF, Apple DF, Burns AS, et al. A View of the Future Model Spinal Cord Injury System Through the Prism of Past Achievements and Current Challenges. J Spinal Cord Med 2003;26:110-115.






